
Automation has become one of the most talked-about topics in healthcare revenue cycle management (RCM). With the hype around AI, many leaders assume they already “have automation” in place. But there’s a big difference between having tools that can automate tasks and knowing what should be automated next — safely, accurately, and without risk to revenue or compliance.
Like the story of King Midas, who discovered too late the danger of turning everything he touched into gold, there’s a cautionary tale in over-automating. In the world of medical coding, the wrong automation decision can mean compliance exposure, lost revenue, or irreparable payer relationships. But the opposite risk is just as real: under-automating. By relying only on human intuition to decide automation priorities, many RCM teams leave massive efficiency gains untapped.
The Twin Risks of Automation
The Risk of Over-Automating
In theory, it sounds appealing to automate everything. But medical coding is full of nuance — context matters, payor rules change, and a wrong decision at scale creates multiplied risk. Automating too aggressively can lead to denials, compliance violations, or systemic underpayments.
Like Midas, the results of “too much automation” may not be what you hoped for.
The Risk of Under-Automating
On the flip side, most human brains naturally gravitate toward “low-hanging fruit” when thinking about automation. Teams can usually identify the obvious 20–30% of repeatable coding tasks that make sense to automate. But beyond that, it gets difficult. Complex patterns and subtle inefficiencies are often invisible without advanced analytics. This leaves significant value unrealized.
Under-automation is safe — but costly.
White Plume’s Approach: Augmented Intelligence, Not Blind Automation
At White Plume, we solve both of these challenges by blending Analytics + AI + Expert Communication:
- Analytics surface the full range of automation opportunities, not just the obvious ones.
- AI identifies patterns across millions of encounters, highlighting where automation can safely and accurately be applied.
- Expert Client Success Teams collaborate directly with RCM leaders to validate and prioritize those opportunities.
This isn’t “AI instead of humans.” It’s augmented intelligence — humans and AI working together to automate what’s safe, scalable, and valuable.
A Real-World Example: From 35% to 55% Automation
One client’s journey illustrates this perfectly.
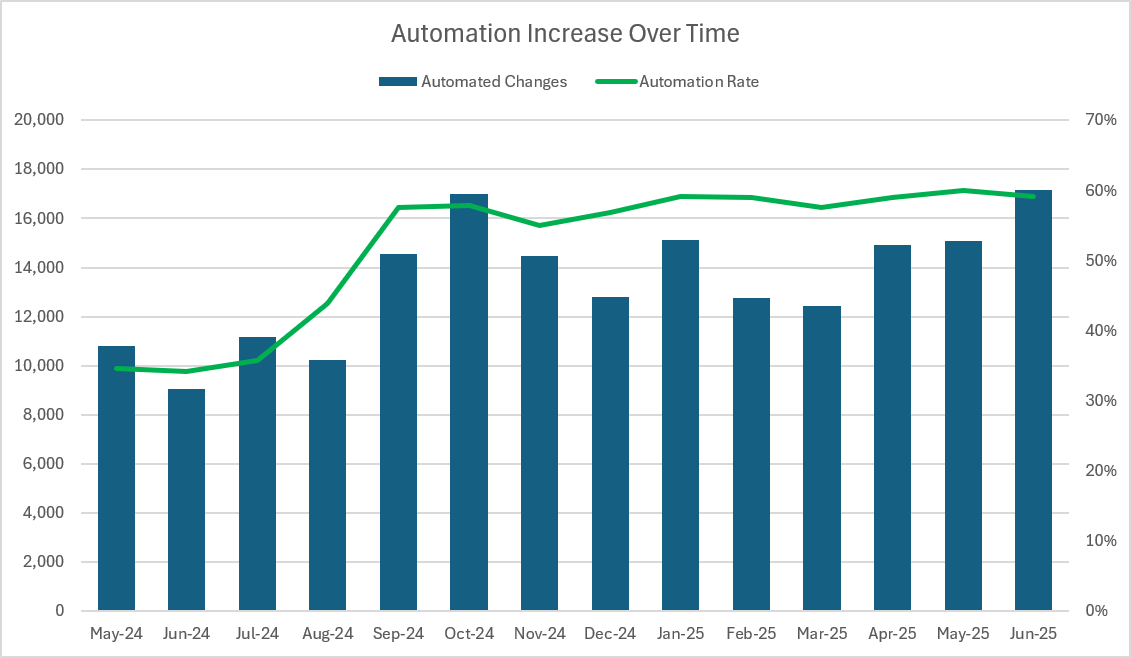
Fig 1. Automation compounds over time and drives medical coding efficiency—each stage builds momentum, creating lasting revenue and productivity gains.
At the start, their team had already identified opportunities to automate roughly 35% of coding and billing changes behind their physicians and EHR. That early win gave them meaningful efficiency gains.
But when paired with White Plume’s analytics and AI-driven insights, the picture expanded. Working collaboratively with their coders, our Client Success team helped surface additional automation opportunities that the human brain alone couldn’t see.
Over time, their automation rate climbed to 55% — safely and accurately. The number of automated changes per month grew from 10,000 to over 16,000, dramatically increasing productivity and revenue capture without sacrificing compliance.
This wasn’t “blind automation.” It was smart, guided, data-driven automation — built on the strengths of people and AI working together.
The Takeaway: The Power of Knowing What’s Next
The question in RCM isn’t simply “do you have automation?” It’s:
- Do you know what should be automated next?
- Are you avoiding both the risks of over- and under-automation?
- Are you leveraging analytics, AI, and expert insight together to keep moving forward?
White Plume’s approach ensures that the next automation decision is always the right one. The result is safer workflows, higher revenue integrity, and continuous improvement over time.
Ready to see where your automation rate could grow next? Book a demo today and let’s explore your opportunities together.




